Have you ever wondered what happens to your brain in outer space?
On earth, the force of gravity1 holds our bodies together and keeps us on the ground. Out in space, the force of gravity is limited, a condition known as microgravity2. Microgravity affects the human body in many ways, some of which we already know. For example, microgravity can weaken our bones and muscles, which need the force of gravity to maintain their strength. However, the amount we know about the effects of microgravity on the human body pales in comparison to what we don’t know.
To understand how microgravity may affect the brain, Dr. Jeanne Loring, Professor Emeritus in the Department of Molecular Medicine3 and Founding Director of the Center for Regenerative Medicine4 at Scripps Research Institute in San Diego, CA, and colleagues sent brain cells to space, where they spent a month on the International Space Station5.
Dr. Loring hopes that this research will help us better understand the effects of microgravity on the brains of astronauts, as well as understand the impacts of brain diseases for the rest of us living here on Earth.

Figure 1.
International Space Station, with Earth in the background.
[Source: https://www.nasa.gov/reference/international-space-station/]
Working with Stem Cells
According to recent estimates, a 70-pound, 10-year-old human child is made up of approximately 17 trillion cells, and human adults almost double that. These cells are the building blocks of all the organs and tissues in our bodies, and they share genetic material in common.
All cells begin as stem cells6, no matter the function they will eventually serve in the body. Stem cells are unique because they can reproduce themselves and they are unspecialized cells. Their ability to reproduce means that researchers can continually use stem cells that are derived from the same group of identical cells, also known as a cell line. As unspecialized cells, stem cells are able to become different types of cells in the body through a process known as differentiation.
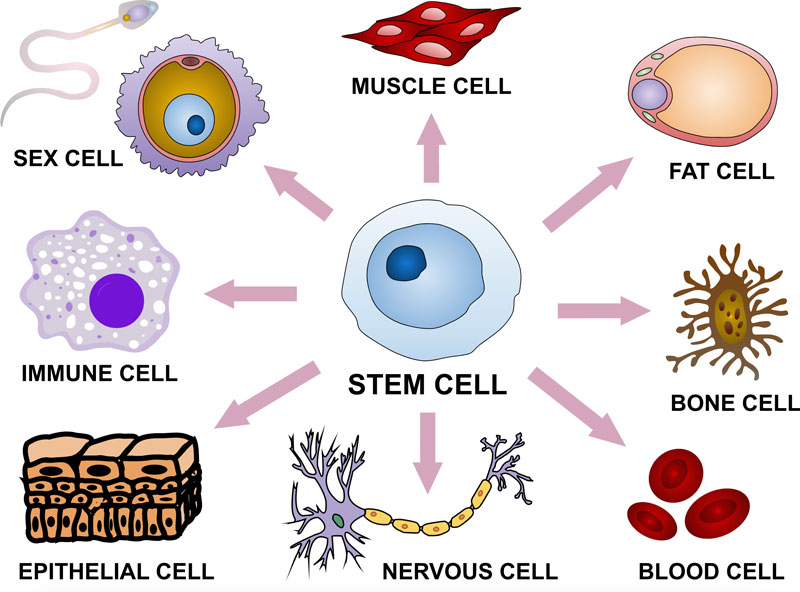
Figure 2.
Stem cells are able to become many different types of cells in the body through a process called differentiation.
[Source: https://commons.wikimedia.org/wiki/File:Stem_cell_differentiation.svg]
Adults have limited numbers of stem cells in certain organs such as the skin, teeth, and blood vessels, that allow those tissues to repair and replace cells that are lost. These stem cells can only become a certain kind of cell. For example, a stem cell in the skin can differentiate into different types of skin cells but cannot become a tooth cell or a blood cell. In contrast, developing embryos contain stem cells that can differentiate into any tissue throughout development, called embryonic stem cells.
Embryonic stem cells may hold the key to treating and reversing many kinds of diseases caused by the loss of different cell types. To generate embryonic stem cells, researchers have developed a technique to reprogram adult stem cells back to their embryonic form. These stem cells are called induced pluripotent stem cells 7 (iPSCs), and they are used by researchers around the world who are seeking to better understand health and disease.
iPSCs are so beneficial because they can be used to create many different cell types, but they can also be challenging to work with. The process of cell differentiation is complex, involving factors both within and outside the cellular environment. To transform a cell from an iPSC to a differentiated cell requires many steps. Each type of cell may require different conditions for differentiation to occur. This process can take years of research to optimize.
Using Stem Cells to Treat Parkinson’s Disease
Dr. Loring has spent her career working with stem cells, and she has worked with iPSCs since their discovery nearly 20 years ago. For much of that time, she has used iPSCs to study Parkinson’s disease8 with the goal of developing new treatments.
Parkinson’s disease is a brain disease characterized by the loss of control of voluntary movements. People with Parkinson’s disease may have trouble with balance and coordination, and they may have symptoms such as shaking and stiffness. Symptoms worsen over time, and people with Parkinson’s disease eventually have more and more difficulty walking and talking. Some may develop dementia. Treatments are available to manage some symptoms of Parkinson’s disease, but there is currently no known cure for the disease.
Parkinson’s disease is caused by the loss of a specific type of brain cell that produces the chemical messenger dopamine9, called dopaminergic neurons. Dr. Loring hypothesized that technology based on iPSCs might offer a treatment strategy for Parkinson’s disease by replacing dopaminergic neurons that were lost. To do that, she spent many years trying to figure out how to make iPSCs into dopaminergic neurons. Testing in cells moved into testing in animal models, and the replacement dopaminergic neurons Dr. Loring developed are now under evaluation in clinical trials for people with Parkinson’s disease.
Brain Cells in Space
Dr. Loring’s vast expertise in stem cells came in handy when she was approached with an opportunity to send stem cells into space. The International Space Station is located 250 miles above the Earth in what is called low-Earth orbit. Researchers at the National Aeronautics and Space Administration (NASA) were interested in the possibility of studying brain cells on the International Space Station because they have no other way of knowing how microgravity might affect the brains of astronauts living there. The research also had the potential to expand our understanding of the brain and brain diseases. “I have always been a novelty seeker,” explained Dr. Loring, “and this was an opportunity I couldn’t pass up.”
When the opportunity presented itself, Dr. Loring had to work quickly, because she and colleagues had only one month to prepare their specimens. The researchers used four lines of iPSCs: two from healthy adults, one from someone with Parkinson’s disease, and one from someone with progressive primary multiple sclerosis10, a brain disease that affects a different type of brain cell called cortical neurons. The cells that initiated these stem cell lines were either obtained during a biopsy, when a sample of tissue is removed from the body, or isolated from urine. The researchers chose these cell lines because they were already available in their laboratories.
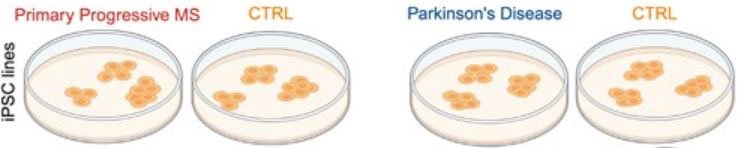
Figure 3.
Dr. Loring and colleagues used four iPSC lines to develop cells to send to space, two from healthy controls, one from someone with primary progressive multiple sclerosis (MS), and one from someone with Parkinson’s disease.
[Source: Marotta et al 2024, Fig 1a]
The researchers relied on their previous experience with stem cells to generate clumps of brain cells, called organoids. They decided to keep each organoid small, about half of one millimeter in diameter. In the brain, neurons are never farther than a half millimeter from a blood vessel, which delivers oxygen and nutrients and takes away waste and carbon dioxide. Similarly, if the organoids had been any larger, the cells in the center would have died from lack of nutrients. In addition, the size the researchers chose was just big enough for the researchers to analyze each organoid for gene expression.
From each iPSC line, the researchers created pre-differentiated neurons called neural progenitor cells and pre-differentiated microglial cells called microglia11 progenitors. Microglia are cells of the immune system found in the brain that are involved in the creation of connections between neurons. Dr. Loring hypothesized that the organoids might develop better with the addition of microglia cells. To make the organoids, the researchers placed the neural progenitor cells in test tubes with a culture medium that helps cells grow. The researchers added microglia to half of the organoids for comparison.
Sending cells into space presented Dr. Loring and colleagues with unique challenges. The organoids would be on the International Space Station for a month. Under normal circumstances, most cells that were left alone for a month would just die. Dr. Loring wanted to make sure the cells would survive. Through a process of trial and error the researchers found the right storage container for the stem cells. Eventually the researchers decided to use test tubes that could be frozen, called cryovials, as these had tight screw-on caps that regular test tubes do not.
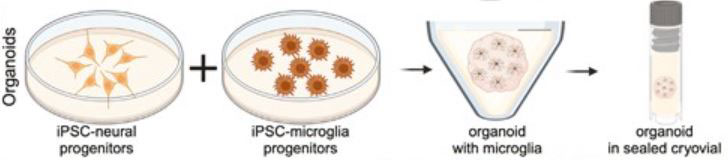
Figure 4.
The researchers developed organoids from iPSC neural progenitor cells that were stored in sealed cryovials. Half of the organoids also contained iPSC microglia progenitors.
[Source: Marotta et al 2024, Fig 1b]
The researchers kept 22 organoids on Earth as controls and sent 20 organoids into low Earth orbit on the International Space Station.
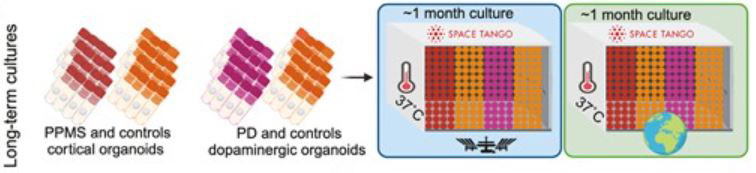
Figure 5.
The researchers developed organoids using stem cells from two healthy controls, one person with primary progressive multiple sclerosis (PPMS) and one person with Parkinson’s disease (PD). Half of the organoids were sent to the International Space Station and half stayed on Earth as controls.
[Source: Marotta et al 2024, Fig 1c]
The Effects of Microgravity on the Brain
When the organoids returned to Earth after a month in microgravity, the first thing Dr. Loring and colleagues wanted to know was whether they had survived the trip. “Our first discovery was that all of the organoids were still alive and healthy,” commented Dr. Loring.
Next, the researchers performed tests on both the control organoids that stayed on Earth and the experimental ones that went to space to understand how microgravity may have affected them. Some of these tests involved visualizing the cells and observing changes.
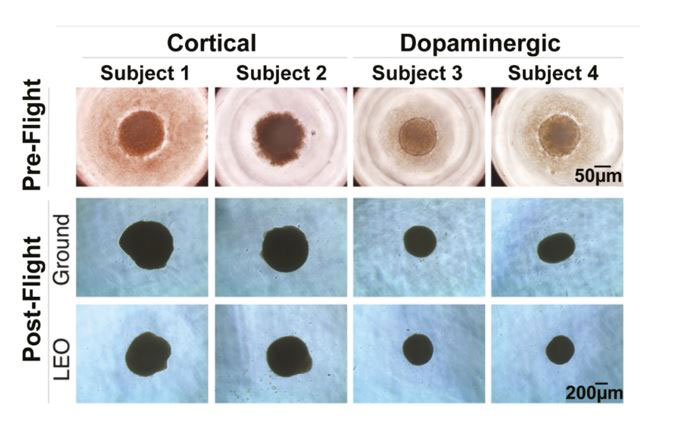
Figure 6.
Images of cortical and dopaminergic organoids that stayed on Earth (ground) and went to space (LEO) from each of the four iPSC cell lines before and after the space mission.
[Source: Marotta et al 2024, Fig 2a]
The researchers noted enhanced growth of neural fibers in the organoid cells that went to space.
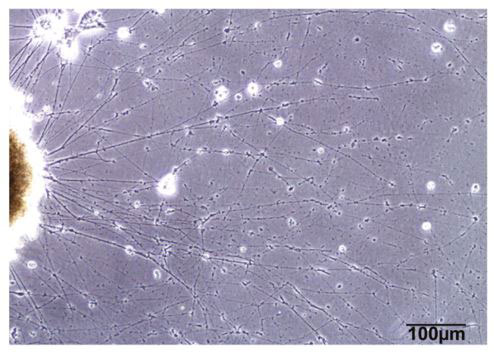
Figure 7.
Enhanced neural fiber growth in the organoids that went to space.
[Source: Marotta et al 2024, Fig 2b]
They noticed changes in protein expression in the cortical organoids before and after space. Some of these changes were observed only in the organoids that contained microglia.
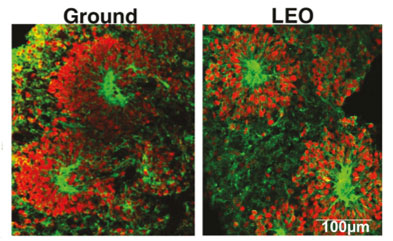
Figure 8.
Protein expression of two common proteins in cortical neurons differed between the organoids that stayed on Earth (ground) and those that went to space (LEO).
[Source: Marotta et al 2024, Fig 2c]
The researchers also tested the expression of genes and proteins in the organoids to look for differences between those that went to space and those that stayed on Earth. In particular, they were interested in how microgravity might affect the immune system and inflammation of brain cells, as inflammation is involved in most brain diseases.
The researchers identified 1,183 genes that were different in the dopaminergic organoids that went to space compared to the ones that stayed on Earth, and 926 genes that were different between the two groups of cortical organoids. “The huge number of genes that were different between the organoids that stayed on Earth and those that went to space indicate that microgravity had a significant impact on the cells,” commented Dr. Loring.
The researchers performed additional testing to better understand how these differentially expressed genes might affect the organoids. Surprisingly, they did not find signs of stress or inflammation in either group, though the cells that stayed on Earth had elevated levels of genes associated with stress compared to those that went to space. In addition, the researchers found an increase in markers associated with cell differentiation and a decrease in genes associated with cell growth in the cells that went to space, meaning that the cells matured faster and grew less.
These results are from the first mission that sent organoids into space. Since then, Dr. Loring and colleagues have done similar experiments four times. With each repetition, they follow similar protocols with additional changes based on previous findings. One of the organoids sent to space was derived from Dr. Loring’s own stem cells. “I have the honor of probably being the first scientist who has sent their cells into space,” remarked Dr. Loring.
In future missions, Dr. Loring would like to study additional areas of the brain, including those affected by other brain diseases such as Alzheimer’s disease12 and Huntington’s disease13. The researchers have also updated their protocols and asked the astronauts to assist them in observing the organoids. They have access to a digital microscope, which allows the researchers to stay on Earth and observe the cells in space. In the latest missions, the researchers added a fluorescent protein to the organoids that would let them know when a neuron had matured. “We’re excited to see where this takes us,” added Dr. Loring. “When you follow your curiosity, the sky is the limit.”
Dr. Jeanne Loring is Professor Emeritus in the Department of Molecular Medicine and Founding Director of the Center for Regenerative Medicine at Scripps Research Institute in San Diego, CA. She has spent her career working with stem cells with a particular focus on Parkinson’s disease and other neurodegenerative diseases. Outside the laboratory, one of Dr. Loring’s favorite hobbies is traveling the world to view total solar eclipses. She saw her first total solar eclipse while still in graduate school and has seen a total of 16 to date.
For More Information:
- Marotta D, Ijaz L, Barbar L, et al. Effects of microgravity on human iPSC-derived neural organoids on the International Space Station. Stem Cells Transl Med. 2024;13(12):1186-1197. doi:10.1093/stcltm/szae070. https://academic.oup.com/stcltm/article/13/12/1186/7833382
To Learn More:
Stem Cells
- Loring laboratory. https://www.scripps.edu/loring/index.html
- National Institutes of Health. https://stemcells.nih.gov/info/basics
Parkinson’s Disease
- National Institute on Aging. https://www.nia.nih.gov/health/parkinsons-disease
- Parkinson’s Foundation. https://www.parkinson.org/
Multiple Sclerosis
- National Institute of Neurological Disorders and Stroke. https://www.ninds.nih.gov/health-information/disorders/multiple-sclerosis
- National Multiple Sclerosis Society. https://www.nationalmssociety.org/
Space Research
- International Space Station. https://issnationallab.org/space-for-everyone/
- “The Human Body in Space.” National Aeronautics and Space Administration. https://www.nasa.gov/humans-in-space/the-human-body-in-space/
Written by Rebecca Kranz with Andrea Gwosdow, PhD at www.gwosdow.com

