| |
What do peanuts and pollen have in common? You guessed it! They're both common
allergens
- substances that cause
allergic reactions
in susceptible individuals. According to the Asthma and Allergy Foundation of America, approximately 50 million Americans - that's one in five -
suffer from some sort of allergy.
Allergic reactions can range from a very mild (but annoying) runny or stuffy nose to extreme reactions that can lead, in severe cases, to
anaphylactic shock
or even death.
In order to keep us healthy, our immune cells must correctly distinguish between harmless agents and potentially harmful ones.
You may be wondering: How can compounds so common in the environment lead to such extreme reactions? The answer lies in the protective mechanisms of the
immune system,
a network of different types of cells throughout the body that work together to prevent and fight infection. In order to keep us healthy, immune cells must correctly distinguish between harmless agents and potentially harmful ones. In general, an allergic reaction occurs when the immune system makes a mistake. It starts attacking agents that aren't actually harmful - peanut residues, pollen spores, and other allergens. In the last decade, scientists around the world have begun investigating the relationship between allergic reactions and cancer. Now, researchers from King's College in London have found evidence suggesting that allergic reactions in the skin may actually protect against cancer.
Let's be clear: the researchers this month were focused on a very specific allergic reaction -
atopic dermatitis
- and its relationship to a particular type of cancer - skin cancer. Atopic dermatitis, more commonly known as eczema, is an allergic condition that affects somewhere between 10 and 30 percent of the population in the United States,
according to the National Institutes of Health.
It generally begins in childhood, before age five, and can persist into adulthood.
Children with atopic dermatitis develop red patches on the arms, face, or behind the knees. These patches can become so itchy that patients can't sleep. Scratching inflames the dermatitis (making it itchier), and once the skin barrier is broken it becomes much easier to develop infections.

Picture of a skin region affected by atopic dermatitis.
"Essentially, it's your immune system on overdrive."
Patients who go to the doctor's office with atopic dermatitis are told to avoid certain creams and soaps and are given some ointments to reduce the symptoms. In severe cases, they are put on medications that regulate the immune system. Why the immune system? Atopic dermatitis is caused by sensitive skin plus, like most allergic reactions, an exaggerated immune response. "Essentially, it's your immune system on overdrive," explained Dr. Sara Cipolat. "And we wanted to figure out why," added her colleague Dr. Esther Hoste. Drs. Cipolat and Hoste are researchers in the laboratory of Dr. Fiona Watt at the Centre for Stem Cells and Regenerative Medicine at King's College in London, England, where the study was conducted.
To begin their research, Drs. Cipolat and Hoste and a team of colleagues began with a mouse model that lacked the genes for three proteins--
envoplakin,
periplakin,
involucrin
--involved in the skin's barrier function of protecting the body. These mice are called
"triple knock-out" mice
because these three genes have been "knocked-out," or removed, from the
genome.
Previous studies had shown that mice lacking these proteins would develop red, itchy patches on their skin similar to patients with atopic dermatitis. The researchers wanted to know what would happen to the knock-out mice with atopic dermatitis if they were also to develop skin cancer.
To find out, they treated a group of knock-out mice and a group of control mice with a combination of two chemicals known to induce tumor formation in the skin. The first chemical (7,12-dimethylbenz(a)anthracene, or DMBA for short) causes
genetic mutations
in skin cells. The second chemical (12-O-tetradecanoylphorbol-13-acetate, or TPA) stimulates the immune system and causes the cells with DMBA-caused mutations to form
benign
tumors also called papillomas, some of which may eventually become cancerous
squamous cell carcinomas,
a common form of skin cancer affecting the cells in the outermost layer of skin.
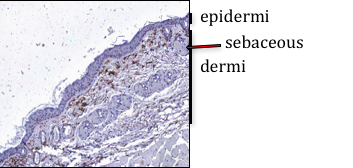
Microscopic image of mouse skin treated with inflammatory chemicals. Immune cells are stained brown, other cells are blue.
Indeed, the researchers found that the knock-out mice developed five to six times fewer tumors than the control mice with the same treatment. But when the knock-out mice did develop tumors, they were more likely to be very nasty cancers.
After treating the mice for 16 weeks with these two chemicals, the researchers removed the skin tumors that had formed for further analysis. "The results of these experiments were striking," explained Dr. Hoste. "Yes," Dr. Cipolat laughed, "the findings were not subtle." Indeed, the researchers found that the knock-out mice developed five to six times fewer tumors than the control mice with the same treatment. But when the knock-out mice did develop tumors, they were more likely to be very nasty cancers-more invasive and more likely to metastasize (or spread). "There was clearly something about the missing genes in the knock-out mice that enabled them to effectively prevent and reduce tumor formation," explained Dr. Cipolat.
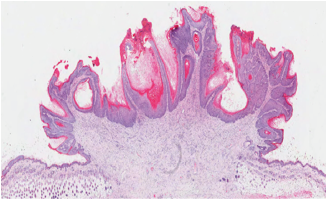
Microscopic image of a papilloma or benign tumor.
To better understand the protective mechanisms of the knock-out mice, Drs. Cipolat and Hoste re-did the same experiments, but this time with only one chemical at a time. Using the same experimental design, the researchers first treated the two groups of mice with only DMBA, the chemical that causes potentially cancer-forming mutations in skin cells. They observed no difference in tumor formation between the two groups. This indicated that the striking differences in tumor formation observed with the combined DMBA-TPA treatment were not related to the mechanisms of genetic mutation. In other words, the skin cells of both the knock-out mice and the normal mice were equally susceptible to the genetic mutations caused by DMBA.
The researchers next moved to TPA, the inflammatory agent, to try to explain the differences in tumor formation. They re-did the previous experiment, this time treating the two groups of mice with only TPA. TPA initiated an extreme inflammatory response in the knock-out mice compared to the control mice. To understand why, the researchers attempted to block the inflammatory response by using compounds known to inhibit particular molecules or cell types involved in the immune response. In this way, they identified two molecules that drive the immune response caused by TPA treatment: TSLP and NKG2D.
Thymic stromal lymphopoietin, or TSLP, is an immune
signaling molecule
released by particular skin cells called
keratinocytes.
NKG2D is a protein found on the cell membranes of immune cells in the skin. Both of these molecules are involved in the exaggerated immune response of skin cells in atopic dermatitis. When keratinocytes are inflamed, they release TSLP, which stimulates a
receptor,
NKG2D, and this cross-talk initiates a cascade of events in the inflammatory response.
To verify their results, the researchers conducted an additional series of experiments blocking either TSLP or NKG2D in the knock-out mice. Recall that the knock-out mice lack three genes so that, without any treatment, they will develop symptoms similar to that of humans with atopic dermatitis. When treated with antibodies that inhibit TSLP, however, the atopic dermatitis was significantly reduced. Treatment in which NKG2D was blocked had similar results, although to a lesser extent. These results confirmed that both TSLP and NKG2D are involved in the immune response that causes atopic dermatitis in mice. "Our results indicate that atopic dermatitis is caused by over-reactive keratinocytes," explained Dr. Hoste.
The keratinocytes will start an immune response against agents that aren't actually harmful to the body.
The researchers hypothesize that genetic factors like those found in the knock-out mice cause the keratinocytes to have a defective barrier. As a result, the keratinocytes will start an immune response against agents that aren't actually harmful to the body. They are activated too frequently, resulting in the red, itchy skin characteristic of atopic dermatitis. As the researchers also found, however, this over-reactive immune response also suppresses tumor formation in the skin.
"We have a lot more work to do and many more leads to follow," Dr. Cipolat commented. On the allergy side, it is interesting to note that TSLP has also been found to be involved in
asthma,
another allergic condition. The researchers want to better understand the role of TSLP and NKG2D in the development of atopic dermatitis, as well as other allergic conditions, in the hope of identifying better treatment options. "We are also very interested in the link between skin cells and tumor formation," added Dr. Hoste. A further area of research is related to the wound healing response and how skin repairs and forms tumors. Both researchers agreed: "We certainly have a lot more work ahead."
Dr. Sara Cipolat is a Research Associate in the laboratory of Dr. Fiona Watt at the Centre for Stem Cells and Regenerative Medicine at King's College in London, England. She was trained as a medical biotechnologist before moving into research. She is originally from Italy and joined Dr. Watt's lab in 2008. Dr. Cipolat recently had twins, so any time not spent in the laboratory or exercising is devoted to her family.
Dr. Esther Hoste is a Research Associate in the laboratory of Dr. Fiona Watt at the Centre for Stem Cells and Regenerative Medicine at King's College in London, England. She obtained her PhD in biology in her native Belgium before joining Dr. Watt's laboratory. In her free time, Dr. Hoste enjoys attending cultural events, running and reading.
To Learn More:
- Cipolat, S. et al. 2014. "Epidermal barrier defects link atopic dermatitis with altered skin cancer susceptibility." eLife, 3.
For More Information:
Atopic Dermatitis
- National Institute of Arthritis and Muculoskeletal and Skin Diseases. www.niams.nih.gov/Health_Info/atopic_dermatitis/default.asp
- National Eczema Association. nationaleczema.org/eczema
- American Academy of Dermatology. www.aad.org/dermatology-a-to-z/diseases-and-treatments/a---d/atopic-dermatitis
- Mayo Clinic. www.mayoclinic.org/diseases-conditions/eczema/basics/definition/con-20032073
Allergies
- National Institute of Allergy and Infectious Diseases. www.niaid.nih.gov
- Asthma and Allergy Foundation of America. www.aafa.org
- Allergy and Asthma Network. www.aanma.org
Skin Cancer
- National Cancer Institute. www.cancer.gov/cancertopics/types/skin
- Centers for Disease Control and Prevention. www.cdc.gov/cancer/skin
- Skin Cancer Foundation. www.skincancer.org
- American Academy of Dermatology. www.aad.org/dermatology-a-to-z/diseases-and-treatments/q---t/skin-cancer
Written by Rebecca Kranz with Andrea Gwosdow, PhD at www.gwosdow.com
HOME | ABOUT | ARCHIVES | TEACHERS | LINKS | CONTACT
All content on this site is © Massachusetts
Society for Medical Research or others. Please read our copyright
statement — it is important. |
|
|

Dr. Cipolat (left) and Dr. Hoste (right) during a conference in Boston, MA, US

In this video, Prof. Fiona Watt discusses skin cancer and stem cells. Prof. Watt's laboratory was the site of the research in this month's What A Year!. http://www.wellcome.ac.uk/About-us/Policy/Spotlight-issues/Human-Fertilisation-and-Embryology-Act/Interviews/WTD040162.htm
Atopic Dermatitis (Eczema)
Here is a brief and clear explanation about the mechanism of atopic dermatitis.
Sign Up for our Monthly Announcement!
...or  subscribe to all of our stories! subscribe to all of our stories!

What A Year! is a project of the Massachusetts
Society for Medical Research.
|
|

