| |
We all know that memory loss is part of growing older.
Your parents can´t remember where they left their keys; your grandparents can´t remember names and dates as well as they used to. For some people, though, memory loss and the loss of other critical thinking skills begins to impede their ability to perform daily tasks and can significantly reduce their quality of life.
Moderate to severe loss of neurological functions in old age is known as
dementia,
a broad term used to describe loss of brain function often associated with other diseases. It is estimated that dementia affects about 1% of the population over 60 years old and 30-50% of those over 85 years old. Dementia is also the leading cause for placing elderly people in nursing homes or other facilities, and in most cases it is an irreversible process that worsens over time.
Between 60% and 80% of all cases of dementia are associated with the condition known as
Alzheimer's disease.
According to the Alzheimer´s Association, approximately 5.4 million Americansabout 1 in 8 Americans over 65 years of ageare currently living with the disease.
Alzheimer´s disease is the sixth-leading cause of death in the United States, and the only cause of death in the top ten that cannot be prevented, cured, or stopped in any way. See facts and figures.
Alzheimer´s disease is perhaps one of the most intensively studied neurological diseases. Nevertheless, we still know extremely little about what causes the disease or how it progresses, key steps to developing any sort of treatment or cure. To understand what we do know, and the latest research being done, let´s start with some brain basics.
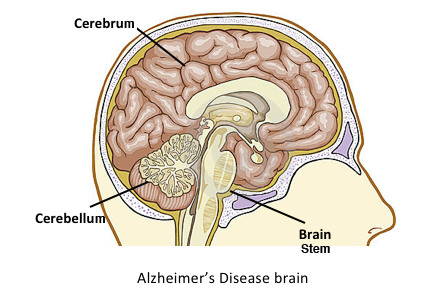
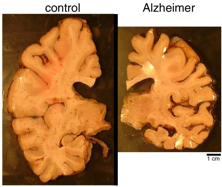
Brain Review
On a macro level, the human brain is composed of three main parts: the
cerebrum, the
cerebellum, and the
brain stem. The brain stem is located at the very base of the skull and attaches to the uppermost part of the
spinal cord. It is responsible for our most basic functions such as maintaining the proper body temperature, heart rate, respiratory rate, and blood pressure. The cerebellum is beneath the cerebrum and accounts for about one tenth of all brain mass. It serves primarily in muscle control and coordination. The largest and most complex part of the brain is the cerebrum, which accounts for over 80% of total brain mass.
The outermost layer of the cerebrum, known as the
cerebral cortex, is responsible for all conscious behavior and is divided into distinct areas based on functionfor example the visual cortex processes visual information, while the motor cortex controls all voluntary movements. The cerebral cortex is about one-quarter inch thick and surrounds the inner white matter of the cerebrum, which is responsible for communication between the different regions of the brain.
There are two primary cerebral regions that are critical for proper memory: the
hippocampus and the
entorhinal cortex (EC).
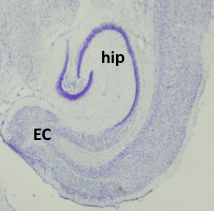 A mouse brain slice showing the entorhinal cortex (EC) and hippocampus (hip).
The hippocampus, located just beneath the cerebral cortex is the primary region of the brain involved in the consolidation of information to form short-and long-term memories. The hippocampus is also involved in our memory of, and ability to navigate ourselves through space. Located directly between the hippocampus and the cerebral cortex, the EC is responsible for communication between the hippocampus, cerebral cortex, and other brain structures to form and maintain memories. Not surprisingly, the EC and the hippocampus are the first structures affected by the abnormalities associated with severe dementia and Alzheimer´s disease.
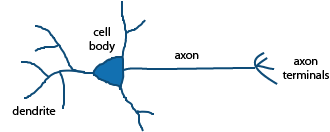
On the micro level, the entire brain and nervous system is composed of specialized nerve cells called
neurons that transmit electrical signals from one neuron to another. The neurons are located within a fluid known as the
extracellular matrix. Both inside the cells and outside in the extracellular matrix are thousands of proteins, structures composed of those proteins, and a variety of other compounds that are critical for proper brain function.
Protein Problems
When even just one of these compounds, structures, or proteins is not working correctly, it can result in a disease state. In the case of dementia and Alzheimer´s disease, there are two main biological features that have been observed in most patients: the accumulation of large amounts of hardened deposits of
amyloid protein fragments, and fibrous tangles of the abnormal protein
microtubule binding protein tau (MAPT).
Amyloid beta peptides are protein fragments of amyloid precursor protein (APP) normally produced by neurons and transported outside the cells in the extracellular matrix. In healthy people, these protein fragments are broken down and eliminated. However, in patients with Alzheimer´s disease the amyloids accumulate, forming hard deposits called plaques between the neurons. Despite decades of research, it is still unclear what role amyloids play in the normal brain or in the progression of Alzheimer´s disease.
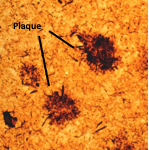 Plaque
Tau is another protein normally produced by neurons that binds to another protein called tubulin to form small tubes known as microtubules. These microtubules are thought to provide critical structural support to the neurons. But the tau found in people with Alzheimer´s disease has an abnormal structure and can no longer bind to
tubulin. As a result, the microtubules fall apart, and tau protein accumulates into a fibrous mess known as
Neurofibrillary Tangles. These Neurofibrillary Tangles are thought to cause the neurons to die, but if they really do and exactly how the abnormal tau causes the progression of Alzheimer´s disease is still unknown.
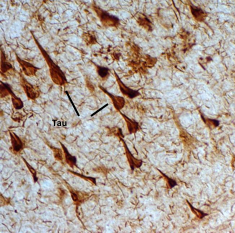 Tau
Of the two proteins, amyloid beta has been the most intensively scrutinized by researchers around the globe. Researchers have tried to reduce the production of amyloid beta, but this approach has not been successful.
More recently, researchers on Alzheimer´s disease have focused their experiments on tau. Imaging studies of patients with mild to moderate dementia and Alzheimer´s disease have established a clear pattern of progression of abnormal tau protein aggregation. For example, in patients with only the beginnings of dementia, the abnormal tau is localized only in the EC. As the disease progresses, more and more tau aggregates can be seen in the EC, the hippocampus and other parts of the brain. In fact, there has even been an index developed to measure the extent of dementia based on the accumulation of tau protein in different regions of the brain.
The Question
The primary question was how the abnormal tau protein got to other parts of the brain. Researchers had two main hypotheses. According to the first hypothesis, the abnormal tau protein actually spreads from neuron to neuron in the same way a bacterial or viral infection might spread from cell to cell. The second hypothesis proposed that some parts of the brain are more resilient to the changes in the tau protein and can resist it for longer periods of time.
For 25 years researchers have tried to explain why abnormal tau aggregates start in a part of the brain and seem to spread to other areas. After years of research, a research team from the Massachusetts General Hospital Institute for
Neurodegenerative Disease developed experiments using a
transgenic mouse model that provide evidence for the transfer of abnormal tau across the brain.
The transgenic mouse model expressed a human mutant tau protein that causes a different type of dementia with similar tau abnormalities to Alzheimer´s disease, but the abnormal protein was only expressed in the ECeverywhere else in the brain had the normal mouse tau protein. The researchers aged these transgenic mice for two yearsextreme old age for laboratory miceand observed the location of the tau protein in the mouse brains at 12, 18, and 24 months of age. They treated the mouse brains with a particular compound that attaches only to the abnormal tau protein and were therefore able to visualize its accumulation in different areas of the brain. ¨The goal of the experiment was to see where the abnormal tau protein was found with age, explains Dr. Manuela Polydoro, a member of the research team.
The human brain pictures are published images but the stages are on this website:http://tau-rx.com/quiz/tangles.html
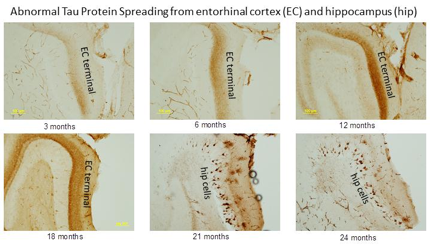
The Result
The researchers found that, over time, the abnormal tau protein followed a similar pattern of spread and accumulation that had been observed in human patients. Even though the mouse model only expressed the abnormal protein in the EC, researchers observed abnormal tau protein build-up first in the hippocampus and then in other regions of the cerebral cortex. Somehow parts of the brain that did not have any abnormal tau were acquiring some! This could only come from the spread of abnormal tau protein.
For Dr. Polydoro and her team, these initial experiments clearly support the first hypothesis for the transfer of tau in the brainthat it is actually spreading like a bacterial or viral infection. This same conclusion was reached independently by a separate research team at The Taub Institute for Research on Alzheimers Disease and the Aging Brain at Columbia University Medical Center, thus corroborating their results.
Dr. Polydoro hopes that the team´s future work will lead to the development of a compound that will block the transmission of abnormal tau and, thus, stop the spread of Alzheimers disease. Their next experiments are aimed at understanding how tau spreads, and correlating this spread with memory loss. The goal of these experiments is to see if the amount of tau protein correlates with the degree of memory loss observed in these mice, explains Dr. Polydoro.
Dr. Manuela Polydoro is a Research Fellow at the Massachusetts General Hospital Institute for Neurodegenerative Disease, in the laboratory of Dr. Bradley Hyman. When she is not in the lab, she spends time with her four-year-old daughter and her husband.
To Learn More:
- de Calignon, A et al. 2012. ¨Propagation of Tau Pathology in a Model of Early Alzheimers Disease.¨ Neuron, 73: 685-697.
- Path is Found for the Spread of Alzheimers New York Times www.nytimes.com/2012/02/02/health/research/alzheimers-spreads-like-a-virus-in-the-brain-studies-find.html, Accessed 16 April 2012.
For More Information:
- MassGeneral Institute for Neurodegenerative Disease. http://www.mghmind.org, Accessed 16 April 2012.
- Alzheimers Disease. http://www.ncbi.nlm.nih.gov/pubmedhealth/PMH0001767/ , Accessed 16 April 2012.
- Alzheimers Disease Fact Sheet. http://www.nia.nih.gov/alzheimers/publication/alzheimers-disease-fact-sheet, Accessed 16 April 2012.
- Alzheimer Research Forum. http://www.alzforum.org/abo/mis/default.asp, Accessed 16 April 2012.
- Alzheimers Association. http://www.alz.org/alzheimers_disease_alzheimers_disease.asp, Accessed 16 April 2012.
Written by Rebecca Kranz with Andrea Gwosdow, PhD http://www.gwosdow.com
HOME | ABOUT | ARCHIVES | TEACHERS | LINKS | CONTACT
All content on this site is © Massachusetts
Society for Medical Research or others. Please read our copyright
statement — it is important. |
|
|
 Research Group
 Propagation of Tau Pathology In a Model of Early Alzheimer's Disease
Sign Up for our Monthly Announcement!
...or  subscribe to all of our stories! subscribe to all of our stories!

What A Year! is a project of the Massachusetts
Society for Medical Research.
|
|

