| |
Highlights
- Lyme disease is caused by an infection with the bacteria, Borrelia burgdorferi, which enters the body by a bite from the blacklegged tick, Ixodes scapularis.
- The process of identifying a single antibody that can protect the body from Lyme disease, called pre-exposure prophylaxis, is described. The next step is large scale antibody production.
- Avoid Lyme disease by tucking your pants into your socks, using insect repellant, and doing a tick check when you come back inside.
Don’t get Lyme disease
Roll up your socks and spray on the insect repellant: the weather is warming up and we’re headed outside! New England is a great place to go outside and explore. Unfortunately, though, the Great Outdoors does not come without health risks. One tiny arachnid in particular has made pants-tucked-into-socks one of the best outdoor fashions: the Deer Tick or Blacklegged Tick, Ixodes scapularis.

Adult female Blacklegged Tick Ixodes scapularis
Source: https://en.wikipedia.org/wiki/Ixodes_scapularis#/media/File:Adult_deer_tick.jpg
Ixodes scapularis is a very small arachnid that inhabits the forests and meadows across New England, especially tall grassy areas. Like mosquitos, Ixodes scapularis feeds off human blood and therefore is capable of transmitting diseases by tick bite. It is important to protect yourself against tick bites by wearing insect repellant. Another popular method of disease prevention is wearing your pants tucked into your socks. This way any ticks that land around your ankles stay on your clothes rather than heading inside to your skin.
Why all the fuss? Because the small, blacklegged tick may carry a very big bite.
Why all the fuss? Because the small, blacklegged tick may carry a very big bite. The most well-known tick-borne disease is
Lyme disease,
an
autoimmune disorder,
which is caused by an infection with the bacteria, Borrelia burgdorferi. The B. burgdorferi bacteria infects a person when the person is bitten by the Blacklegged Tick, Ixodes scapularis.
If left untreated, Lyme disease can spread to the joints, heart and nervous system. Symptoms begin as a fever, headache and fatigue, usually accompanied by a characteristic bulls-eye rash at the site of the tick bite. We mention “usually” because the characteristic rash does not always appear. The classic bulls-eye rash is shown here:
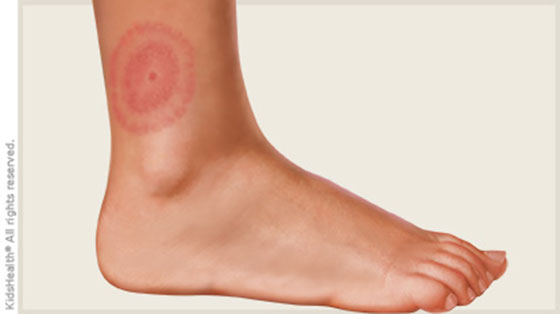
Picture of characteristic bullseye rash
Source: http://kidshealth.org/en/teens/lyme-disease.html#
What can go wrong?
Most cases of Lyme disease can be successfully treated with an appropriate course of
antibiotics.
Nevertheless, even after treatment symptoms may persist. If mild symptoms are not addressed and treated, more serious problems may occur as the disease progresses. Joint pain and
arthritis,
abnormal heart rhythms,
inflammation
of the brain and spinal cord, fatigue, diffuse
musculoskeletal pain
and difficulty thinking often described as feeling like one has “clouded thinking” can all be symptoms of untreated Lyme disease. Damage caused by severe Lyme disease cannot always be reversed, even after proper treatment.
Lyme disease is more a regional problem than a national problem: 96% of cases occur in 14 states in the Northeast and Midwest. Each year about 30,000 cases of Lyme disease are reported to the Centers for Disease Control and Prevention. However, research studies estimate that the actual number of cases is ten times that,
about 300,000 per year.
In addition, these studies indicate that the rates of Lyme disease have doubled between 1991 and 2015.
Global climate change
is a major factor in increasing the risk for Lyme disease and other tick-borne illnesses because shorter winters and warmer weather increase tick habitat and
speed up the tick reproductive cycle.
Like the winter flu, the tick season is here to stay. People living in or visiting areas with a risk of Lyme disease must educate themselves about how to prevent tick bites and how to recognize signs of Lyme disease.
A vaccine?
Health professionals have also been hard at work studying Lyme disease and developing ways to prevent it. In the 1990’s the first
vaccine
for Lyme disease was approved by the Food and Drug Administration. The vaccine was shown to prevent Lyme disease in 78% of cases, but there were problems. The vaccine required three injections over six months ending before the start of tick season. It is difficult to convince people to think about Lyme disease—a summer concern—around Thanksgiving! Second, the vaccine only protected against Lyme disease for one or two seasons. Protection for a second year would require at least one booster injection. Even if people could be convinced to think about protecting themselves or their family from Lyme disease at Thanksgiving, a vaccine that protects for only one or two seasons was very hard to sell and the vaccine was withdrawn from the market in 2002.
MassBiologics focuses on unmet public health needs that are specific to the citizens of Massachusetts, such as Lyme disease.
Lyme disease remains an important public health problem today that many health professionals are working to address. The lessons learned from the vaccine have helped researchers think about developing a better alternative to a vaccine. The latest is an antibody developed under the direction of Dr. Mark Klempner, Executive Vice Chancellor of MassBiologics at the University of Massachusetts Medical School. MassBiologics focuses on unmet public health needs that are specific to the citizens of Massachusetts, such as Lyme disease.
By studying the
host response
to the withdrawn vaccine for Lyme disease, Dr. Klempner gained a better appreciation for the public health challenges involved. In order to convince citizens to immunize themselves, the prevention must
- be a single dose,
- work quickly and
- have few side effects.
- It also must last for at least the duration of one full “tick” season, and it must be affordable.
The first and greatest challenge, though, is biological, namely finding the right antibody to protect the body from Lyme disease.
Vaccine vs antibody
To understand why, let’s compare how a vaccine works and how an antibody works. The basic purpose of a vaccine is to protect the body against a specific infection. Vaccines achieve this goal by introducing a weakened form of the bacteria or virus to the
immune system.
This allows the immune system to recognize particular proteins characteristic of the disease and create specialized proteins, known as
antibodies,
which will fight the infection. However, vaccines don’t only stimulate the production of just the antibody that will prevent disease. Sometimes the vaccine may stimulate the production of antibodies that result in side effects.
Dr. Klempner and his colleagues used a more specific approach. They wanted to identify just the one or two antibodies that afforded protection against Lyme disease and avoid all the extraneous antibodies. Since they are aiming at protecting people from getting Lyme disease they have called their approach pre-exposure prophylaxis, or PREP for short. Unlike a vaccine which stimulates the production of a large cast of antibodies, PREP introduces only the specific antibody needed for protection. It is a more difficult approach because it requires researchers to first identify a single antibody to prevent infection.
The study (Wang et al. 2016) that identified specific antibodies was recently published by Dr. Klempner and his colleagues. These researchers studied mice infected with Lyme disease. The researchers found 593 antibodies involved in fighting Lyme disease. Genetic analysis of all 593 antibodies showed 95 distinct proteins. The researchers took all 95 distinct antibodies to determine which ones were able to kill the Lyme disease bacteria, Borrelia burgdorferi, when introduced into a test tube. Experiments conducted in test tubes are called in vitro experiments.
Each set of test tubes contained a Lyme disease antibody and the Lyme disease bacteria, Borrelia burgdorferi. The test tube contained markers for molecules known as
adenosine triphosphate
or ATP, which provides energy to cells. When the Borrelia burgdorferi die, the cell membrane breaks and releases ATP. The more effective the antibody, then, the more ATP is released and the brighter the test tube becomes. The researchers measured the light intensity in each test tube to determine the most effective antibodies against Borrelia burgdorferi.
The more effective the antibody, then, the more ATP is released and the brighter the test tube becomes.
The first set of experiments narrowed the field, but Dr. Klempner wanted to be more exact. Borrelia burgdorferi causes Lyme disease in the United States but two additional organisms cause Lyme disease worldwide: Borrelia afzellii and Borrelia garinii. In the second and third sets of experiments, Dr. Klempner and team tested antibodies against B. afzellii and B. garinii. After three sets of experiments, 95 potential antibodies were reduced to five.
Dr. Klempner and his team conducted similar experiments to determine which of the five finalists was strongest against all three types of Borrelia bacteria. The greater the light intensity in the test tube, the more bacteria had been killed. These experiments identified a single antibody that was most effective against the Borrelia bacteria.
In vitro to in vivo
The next series of experiments took place in mice. The mice were separated into two groups. One group was given the Lyme disease PrEP antibody; the other was given a random antibody as a control. The following day, the researchers introduced the mice to ticks known to contain Lyme disease bacteria. Three weeks later, the researchers tested the mice for Lyme disease.
The results were impressive. Every single time the researchers conducted this experiment, 100% of mice given the Lyme disease antibody were disease-free while 100% of mice given the irrelevant antibody had Lyme disease. Dr. Klempner found an additional, unexpected result. Not only did the antibody prevent Lyme disease in the mice, it also killed many of the bacteria present in the infected tick.
These experiments were repeated over and over, and each time the researchers reduced the dose of the antibody given to the mice. The goal was to find the minimal dose needed to provide optimal protection.
Results from these experiments showed that the antibody the researchers had identified effectively prevented the transmission of Lyme disease. In order to make an effective Lyme PrEP, though, this protection would have to be long-lasting. Normally, the concentration of these types of antibodies in the bloodstream will decrease by half about every three weeks. This is called the half-life.
In order for protection provided by the antibody to last the entire six month tick season, Dr. Klempner and his team genetically modified the protein, increasing the half-life from 18 to 53 days. This dramatically reduced the amount of antibody needed initially.
After three years of experimentation, Dr. Klempner and his team developed an antibody that might be able to prevent the transmission of Lyme disease from tick to human. They increased the half-life of the antibody and identified the optimal dose to minimize concentration but maximize protection.
The next step is to produce a lot of the antibody for safety testing. Large-scale manufacturing is expensive because antibodies are expensive. Antibodies are made from live cells that must be produced in a sterile environment. Each batch of antibody must be exactly the same and must be purified correctly and efficiently.
Futures
Currently Dr. Klempner and his team are studying ways to improve efficiency in cell production and purification techniques. “This process usually takes a decade,” says Dr. Klempner. “We are well on our way.” Dr. Klempner hopes the antibody for Lyme PrEP will be available to the general public in about 3 to 5 years.
Dr. Mark Klempner is the Executive Vice Chancellor of MassBiologics and Professor of Medicine at the University of Massachusetts Medical School. His research focuses on the development of vaccines and other therapies for infectious diseases like Lyme disease. Dr. Klempner grew up in Miami Beach, Florida, as a self-described “surfer-golf dude.” In high school he had the opportunity to work in a local Veterans Hospital, sparking a lifelong interest in biological science. In addition to his work in the laboratory, Dr. Klempner is an award-winning furniture designer, and has been known to write scientific papers while at work in his furniture studio. He loves spending time outdoors and reminds all students to tuck in their pants, spray on the insect repellant, and get outside! “Just don’t forget that tick check when you come back,” laughs Dr. Klempner.
For More Information:
- Wang Y, Kern A, Boatright NK, Schiller Z, Sadowski A, Ejemel M, Souders CA, Reimann KA, Hu L, Thomas WD, Klempner MS. Pre-exposure prophylaxis with OspA-specific human monoclonal antibodies protects mice against tick transmission of Lyme disease spirochetes. J Infect Dis 2016; doi: 10.1093/infdis/jiw151 http://jid.oxfordjournals.org/content/early/2016/04/16/infdis.jiw151.abstract
- Tang KS, Klempner MS, Wormser GP, Marques AR, Alaedini A. . . Association of Immune Response to Endothelial Cell Growth Factor With Early Disseminated and Late Manifestations of Lyme Disease but Not Posttreatment Lyme Disease Syndrome. Clin Infect Dis. 2015;61:1703-6.
- Souders CA, Nelson SC, Wang Y, Crowley AR, Klempner MS, Thomas W Jr. A novel in vitro assay to predict neonatal Fc receptor-mediated human IgG half-life. MAbs. 2015;7:912-21.
- Klempner MS, Baker PJ, Shapiro ED, Marques A, Dattwyler RJ, Halperin JJ, Wormser GP. Treatment trials for post-Lyme disease symptoms revisited. Am J Med. 2013;126:665-9.
- 5. Klempner MS, Halperin JJ, Baker PJ, Shapiro ED, O'Connell S, Fingerle V, Wormser GP.
Lyme borreliosis: the challenge of accuracy. Neth J Med. 2012;70:3-5.
To Learn More:
- Lyme disease Antibody Eyed. https://www.bostonglobe.com/lifestyle/2015/11/01/findings/D3NjU8T17Q7mlpU0aFnuXL/story.html?utm_medium=email&utm_source=Today-s-Headlines-Brain-Camera-Lyme-Antibody-and-D&utm_campaign=eclipsnov2nd2015
- PrEP for Lyme http://www.bostonmagazine.com/health/article/2015/07/28/massbiologics-lyme-disease/
- Massbiologics http://www.umassmed.edu/massbiologics/
- Lyme disease. http://www.cdc.gov/lyme/
- Patient Information: What to do after a tick bite to prevent Lyme. http://www.uptodate.com/contents/what-to-do-after-a-tick-bite-to-prevent-lyme-disease-beyond-the-basics
- Tick Encounter Resource Center. http://www.tickencounter.org/tick_identification/deer_tick
- Lyme disease. http://kidshealth.org/en/teens/lyme-disease.html#
- 8. Lyme disease, symptoms, pictures and treatment. http://www.medicinenet.com/lyme_disease_pictures_slideshow/article.htm
Written by Rebecca Kranz with Andrea Gwosdow, PhD at www.gwosdow.com
HOME | ABOUT | ARCHIVES | TEACHERS | LINKS | CONTACT
All content on this site is © Massachusetts
Society for Medical Research or others. Please read our copyright
statement — it is important. |
|
|

Dr. Yang Wang

Dr. Mark Klempner

Listen to the radio segment that aired on NPR
Sign Up for our Monthly Announcement!
...or  subscribe to all of our stories! subscribe to all of our stories!

What A Year! is a project of the Massachusetts
Society for Medical Research.
|
|

