Imagine being the participant in your own research study. You want to know: does screen-time before bed affect your sleep? Screen-time includes any time spent in front of a television, computer, smartphone, or any other portable device with a screen like a laptop or tablet. How would you go about performing this study on yourself? How would you measure sleep duration and sleep quality? How would you interpret your findings?
Screen Time, Sleep, and You
New technology is making it easier for individual citizen-scientists to answer these types of questions. When Gregory Marcus, MD, wanted to know how screen-time affected sleep patterns, he opened up his laboratory to everyone in the world with an offer to participate in clinical research. Anyone 18 years or older who was interested and had access to an android smartphone could participate by downloading an app that measured screen-time usage. Specifically, the app measured how many minutes per hour the device screen was open in thirty-day intervals over the course of one year. In addition, participants filled out questionnaires that collected demographic information such as race, gender, and age, as well as medical information including height, weight, physical activity, and sleep habits.
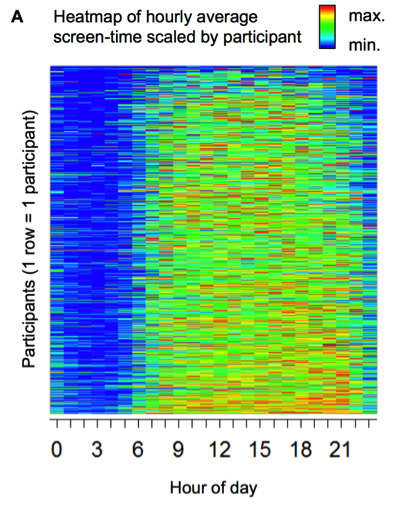
Figure 1. Average amount of screen time over a 24 hour period
Dr. Marcus is Director of Clinical Research for the Division of Cardiology at the University of California San Francisco Medical School, where he is also an Associate Professor and a practicing cardiologist who regularly sees patients. Together with his colleagues, Dr. Marcus has spearheaded a project that uses technology to expand the reach of clinical research. The researchers created the Health eHeart Study to enable anyone 18 years of age or older with an email address to participate in studies to improve heart health and end
heart disease,
the number one cause of death in the United States. Since the Health eHeart Study began, more than 80,000 participants from all 50 states and an additional 50 countries have registered to participate.
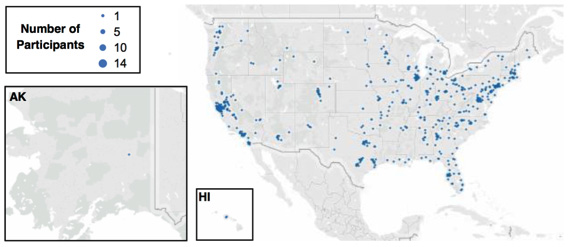
Figure 2. Health eHeart Study participants in the US
It was data from the Health eHeart Study participants that enabled Dr. Marcus to examine the relationship between screen-time and reported sleep habits. He found that, in general, greater screen-time was associated with poorer sleep quality and fewer hours of sleep. In particular, screen-time before bed was associated with longer time required to fall asleep and poorer sleep quality.
It appears from this initial research that screen use interferes with healthy sleep habits. But Dr. Marcus emphasizes that this is not the only way these results can be interpreted. The data suggest a relationship between screen time and sleep habits, but this does not mean that screen time is necessarily influencing sleep habits. It might be the case, for example, that people who have trouble falling asleep – for some other reason unrelated to screen use – happen to use screens more around bed time because they’re having trouble falling asleep. Nevertheless, the findings in this study do support previous research that has shown the potentially adverse effects of screen-use on sleep quality.
Since the Health eHeart Study began, more than 80,000 participants from all 50 states and an additional 50 countries have registered to participate.
So, we come back to our initial question: how does screen-use time affect your sleep? Try it out! Record your normal sleep habits for a few weeks. What time do you go to bed? What time do you wake up? How long do you sleep? How many times do you wake up in the middle of the night? Do you feel rested when you wake up? Now, turn off all screens an hour before you go to sleep for the same time period. Ask yourself these same questions and record your answers. When both phases of the experiment are over, compare your notes. Do you feel different when you don’t use a screen before bed? Do you feel the same? Why might that be? Compare your results with other students in your class. This is science in action.
Second-hand Smoke, Heart Disease, and You
Here’s another interesting question, one that may be more difficult for you to answer alone. This question is of particular interest to Dr. Marcus, who specializes in a heart rhythm disorder called
atrial fibrillation.
Atrial fibrillation is a heart condition where the heart starts beating erratically. This erratic motion can cause
blood clots
to form, which, if released into the bloodstream, can cause a
heart attack
or
stroke.
Dr. Marcus wanted to know about specific risk factors that would make someone more or less likely to develop atrial fibrillation. One such factor that had not previously been studied was exposure to
second-hand smoke.
Cigarette smoke is harmful and potentially dangerous. For the regular smoker, cigarette smoking is associated with higher rates of cancer, especially oral and lung cancer, and heart disease. New research by Dr. Marcus and his colleagues, however, shows that second-hand smoke can be just as dangerous. Second-hand smoke refers to smoke that you inhale even though you yourself are not smoking. The most common form of second-hand smoke exposure is through parents or guardians who smoke regularly.
In order to assess the effects of second-hand smoke exposure on the development of atrial fibrillation, Dr. Marcus and his colleagues invited all participants in the Health eHeart Study to complete a survey of demographic and health information. Nearly 5,000 people did. Some participants were asked about their smoking status, their exposure to second-hand smoke, and whether they had ever been diagnosed with atrial fibrillation.
The findings of this study showed a significant relationship between second-hand smoke exposure and atrial fibrillation. In particular, participants who had been exposed to second-hand smoke while in the womb or during early childhood had a greater likelihood of developing atrial fibrillation many decades later in life. How exactly this happens remains unclear, but one possibility is that exposure to cigarette smoke—either through smoking or inhaling second-hand smoke—alters genetic information that later impacts the heart.
New research by Dr. Marcus and his colleagues, however, shows that second-hand smoke can be just as dangerous as smoking.
Much more research is needed to fully understand the effects of second-hand smoke and the critical periods of exposure. For example, does it matter whether it is the mother that smokes or the father? Does it matter whether the mother smoked during pregnancy if she quits once the child is born? What is the cumulative impact of having two parents who smoke as opposed to one? These are all questions that need to be answered—by the next generation of scientists.
The Future, Technology, and You
Dr. Marcus is excited about the opportunities that are opened when technology enables people from all over the world to participate in clinical research. The number of participants in the Health eHeart Study is growing every day. This information enables Dr. Marcus and his colleagues to ask and seek answers to important health questions like how screen-time affects sleep quality and how second-hand smoke exposure affects heart health. Future research will allow Dr. Marcus to look more closely at the effects of poor sleep on heart rate, mood, and other variables the next day, as well as changes in weight and other health problems that may take longer to develop.
He is working to develop technology to make it easier for individuals to conduct research on themselves, like the studies discussed above. He imagines a network where participants could sign up to investigate the effects of a particular trigger or exposure—like a certain food item, physical activity, or another simple lifestyle modification. Participants would receive instructions on what to do and how to input their information into the database. This would allow individuals to conduct research experiments themselves and enable trained scientists to analyze the entire dataset. The possibilities are endless.
Dr. Gregory Marcus is Associate Professor at the University of California San Francisco School of Medicine and Director of Clinical Research for the Division of Cardiology. He is a trained cardiologist who specializes in heart rhythm disorders. His research focuses on risk factors for the development of atrial fibrillation and other heart problems. Dr. Marcus studied philosophy as an undergraduate student and chose a career in medicine in order to help save lives. When not in the clinic, the classroom, or the laboratory, Dr. Marcus enjoys playing music, sports, and spending time with his family.
For More Information:
- Christensen, Matthew, et al. 2016. “Direct Measurements of Smartphone Screen-Time: Relationships with Demographics and Sleep.” PLoS One 11(11): e0165331.
- Dixit, Shalini, et al. 2016. “Secondhand Smoke and Atrial Fibrillation: Data from the Health eHeart Study.” Heart Rhythm, 13(9): 3-9.
To Learn More:
Heart Disease
- Health eHeart Study.
https://www.health-eheartstudy.org/
- American Heart Association.
http://www.heart.org/HEARTORG/Conditions/Conditions_UCM_001087_SubHomePage.jsp
- Centers for Disease Control and Prevention.
https://www.cdc.gov/heartdisease/
- World Health Organization
http://www.who.int/cardiovascular_diseases/en/
Secondhand Smoke
- American Cancer Society.
http://www.cancer.org/cancer/cancercauses/tobaccocancer/secondhand-smoke
- National Cancer Institute.
https://www.cancer.gov/about-cancer/causes-prevention/risk/tobacco/second-hand-smoke-fact-sheet
- U.S. Department of Health and Human Services.
https://betobaccofree.hhs.gov/health-effects/secondhand-smoke/
- American Lung Association.
http://www.lung.org/stop-smoking/smoking-facts/health-effects-of-secondhand-smoke.html
Technology and Sleep
- National Sleep Foundation.
https://sleepfoundation.org/ask-the-expert/electronics-the-bedroom
- Sleep.org.
https://sleep.org/articles/how-technology-changing-the-way-we-sleep/
- Sleep Health Foundation.
https://www.sleephealthfoundation.org.au/public-information/fact-sheets-a-z/802-technology-sleep.html
Written by Rebecca Kranz with Andrea Gwosdow, PhD at www.gwosdow.com

